As a licensed social worker with Baptist Health Systems, I spend my days with people who are having some of their toughest days. They may be sick, but over time I’ve come to learn that what’s happening to their bodies is not their hardest challenge.
Here are a few things I wish everyone knew about people and healthcare:
People don’t simply choose their way into disease.

In the healthcare field, we talk a lot about “medical non-compliance” when patients don’t adhere to what medical providers are recommending, like following a heart-healthy diet or monitoring your blood glucose level.
Sometimes a moral stigma is attached to non-compliance, as though patients are simply choosing to make poor decisions, and chronic illness is the consequence. Perhaps this is true for some people, but certainly not the majority.
For many people, healthier living costs more than they can bear. By any standard, food has continued to become more expensive, and in areas of our city where people have lower incomes, you’ll find there are generally fewer grocery stores. In those grocery stores, you’ll also find there is less variety of fruits and vegetables.

Produce Vendor at Pearl Brewery.
Medications like insulin or anticoagulants are no different. A leading brand name medication used to treat blood clots retails for $594 for a one-month supply without insurance. With health coverage, I still see copays that are $50, $100, $200–prices that are a significant burden for many of us. For those who may be living off $700 per month in Supplemental Security Income, and who must feed themselves or help feed others with that much money, what we think of as a “healthy lifestyle” simply isn’t an option.
To receive medical care, you have to be able to get to it.
Think about all the appointments we must juggle when managing an illness: clinics, blood draws, radiological imaging, pharmacies, follow-ups, etc. Staying healthy is time-consuming even when all your resources are within a short driving distance.
But for those living in healthcare deserts, such as on our city’s Southside, transportation can be a major barrier. Assuming they are physically able to use the city bus system, a patient traveling from the Madla Transit Center on the Southside would have to travel about fifty minutes, one way, to arrive at a major medical center near downtown.

Pedestrian exits VIA bus on South Flores on the Southside of San Antonio.
For some, that is fifty minutes of unpaid leave or fifty minutes that they must find care for their children. Others must rely on the availability of family or friends, who may or may not be able to take time from their jobs and other responsibilities.
Health happens in community.
In 2019, the San Antonio Express News cited a study using over 1 million Texas birth and death certificates to predict life expectancy by ZIP code. In San Antonio, there was a twenty-year difference between the ZIP code with the highest life expectancy, 78254, and the lowest, 78208.
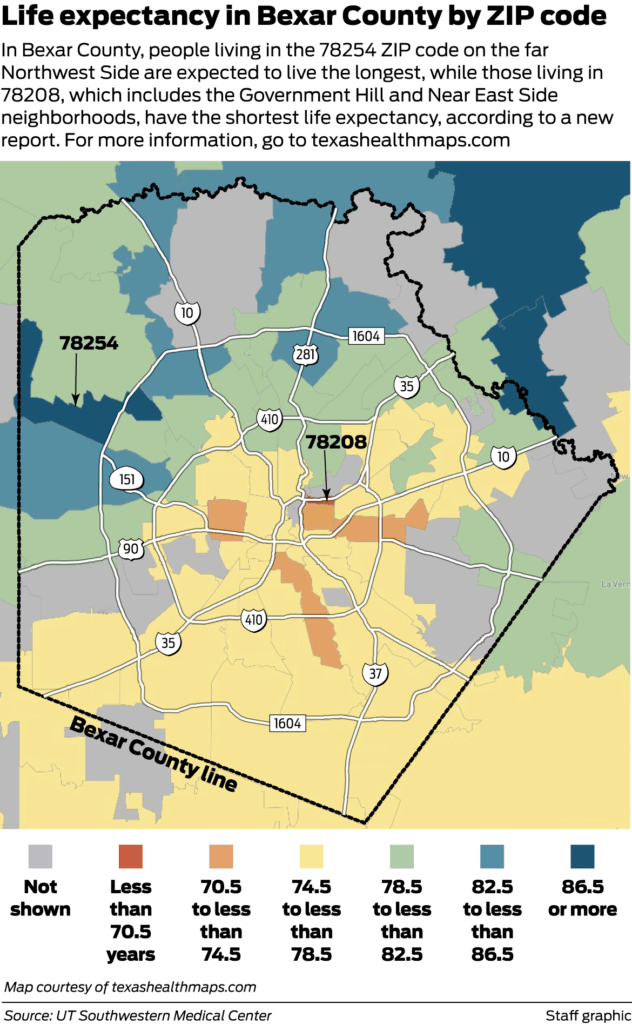
In healthcare, we often talk about risk factors—factors that contribute to poor health outcomes. For San Antonians, a major risk factor is the ZIP code in which you live. Because San Antonio is so economically segregated, it would be easy to live an entire life in our city without seeing the risk factors that nearly 18% of our neighbors experience.
In social work, we also examine protective factors, one of which is community. Almost every day, I get to see what is possible when people, despite having few resources, link arms in order to solve a problem. This might be a patient’s family pitching in to help pay for a prescription or a neighbor volunteering to do a grocery run.
Healthcare is a huge problem to solve, especially in San Antonio, but community is almost always the protective factor that removes the barriers to accessing healthcare. I can only imagine what problems we could solve if we created more communities that crossed over highways, railroad tracks, and the outlines of our own ZIP codes.